Newborn Pulse Oximetry Trial
Starship Foundation Funds Life-Saving Pulse Oximetry Trial For Early Dectection Of Congential Heart Defects in Newborns.
National children's hospital Starship, in conjunction with the Liggins Institute, University of Auckland, is launching a pilot programme in April 2016 that has the potential to save lives and improve health outcomes for New Zealand babies born with congenital heart defects.
With significant funding provided by the Starship Foundation, the pilot will introduce pulse oximetry screening of newborn babies as a tool to help detect critical congenital heart defects (CHD), the most common birth defect. Starship is the only hospital in New Zealand with on-site paediatric cardiac specialist services and facilities for paediatric cardiac intervention.
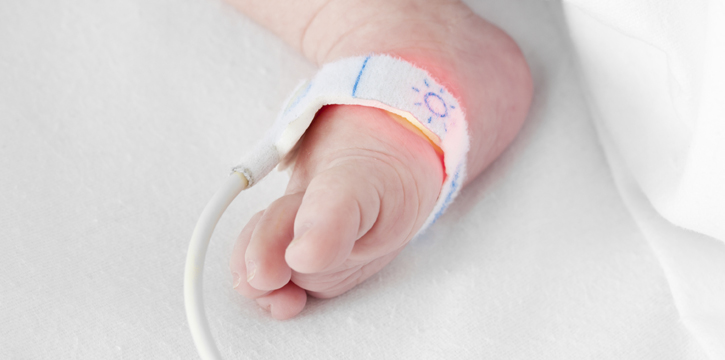
An infant pulse oximeter is a small Band-Aid-like wrap that is placed around the baby's foot, with a light sensor inside that measures oxygen saturation of the blood. It is a simple, non-invasive test that can be completed in a matter of minutes.
The pilot will see all babies born at Auckland City Hospital, or delivered under midwives and delivery units affiliated with the ADHB, offered a pulse oximetry test. Infants not achieving the predetermined oxygen saturation threshold will be referred for a paediatric clinical assessment.
Importantly, the second phase of the trial will roll out later in the year to incorporate pulse oximetry testing for babies born at Counties Manukau DHB facilities, engaging a broader cross-section of the population in a wider array of clinical settings. This has been made possible thanks to valuable funding and support from the Middlemore Foundation for Health Innovation.
Following assessment of the pilot, recommendations will be made regarding the feasibility of establishing a national screening programme for all new-born babies.
CHD affects between four and ten per thousand live-born infants, and is a leading cause of infant death, accounting for more deaths than any other type of malformation. Many CHD babies require cardiac surgery immediately after birth or within their first year of life.
In New Zealand the national standard for CHD screening is via antenatal ultrasound and physical examination at birth. However, some babies born with an undetected heart defect may not display any physical symptoms until 24 hours or more post birth, often then presenting with 'blue baby syndrome' from the lack of oxygen in the blood. There is regional and socioeconomic variability with the current testing; the ultrasound method picks up, on average, just 45% of critical congenital heart defects for New Zealand-born babies.
A recent review estimated 15 New Zealand-born babies a year will receive a late diagnosis of critical CHD, and that four will die as a result. Pulse oximetry screening would likely have detected 50% of these infants with a late diagnosis of critical CHD, with early intervention decreasing the risk of permanent disability or death.
Maximal sensitivity for the detection of CHD can be achieved by combining pulse oximetry with current screening strategies, namely antenatal ultrasound and newborn physical examination. Pulse oximetry screening has a low false positive rate.
Professor Frank Bloomfield, Neonatologist for ADHB, Director of the Liggins Institute and Professor of Neonatology at the University of Auckland, explains: "Early detection of a congenital heart defect gives us the best chance to save a baby's life, and/or greatly reduce the impact on a child's quality of life. Non- or late-detection can severely compromise the cardiovascular system, with significant long-term effects on neurodevelopment.
"This pilot will be an important step towards the realisation of a national screening standard that will improve the outcome of those babies who are born with cardiac abnormalities."
New mum, <name> who had her baby yesterday/ this morning was shown the new technology and had the opportunity to trial the pulse oximeter and reported the test was quick, straight-forward, and hassle free.
"It is reassuring as a new parent to have this test available to help rule out potential heart complications at birth," she said.
Overseas research also indicates pulse oximetry is a valuable clinical tool for detecting congenital heart defects. Successful national screening programmes are in place in Switzerland, Sweden, Norway and the USA, and currently being introduced in the UK.
Professor Bloomfield says while the evidence for setting up national screening is favourable, it first needs to be tested in various environments and communities locally, including hospital, birthing suite and home birth settings, to identify any issues particular to New Zealand with our midwifery-led model of maternity care. "We cannot assume that a screening programme that works with other models of care can simply be transposed to New Zealand without verifying this carefully through a feasibility study," he says.
Pilot funding from the Starship Foundation includes the purchase of 30 Masimo Rad-5 Pulse Oximeters, consumables and the development of resources to initiate the screening pilot at the ADHB. This includes the development of screening guidelines and educational resources for medical staff and parents.
Starship Foundation Chief Executive, Brad Clark, says; "Together with the A+ Trust and Middlemore Foundation for Health Innovation, the Starship Foundation has raised the bulk of the funds required to establish this important pilot at the ADHB and CMDHB. It is an exciting development that will go a long way to mitigating the impact on babies and families affected by a late diagnosis of critical congenital heart disease. We hope it will pave the way for pulse oximetry screening of all New Zealand-born babies as a national standard in the near future."
For further information on the pulse oximetry pilot programme, please visit: /for-health-professionals/starship-clinical-guidelines/p/pulse-oximetry-screening-in-the-newborn/.

